The Bug Zapper
The nightmare woke me at 1:44 in the morning.
I felt the kick first—a jolt to my left side, electrical charge coursing through my chest, my arm, my head. I came up out of sleep certain it had happened. Certain the ICD had fired.
It hadn’t. The nurses pulled several minutes of EKG records to confirm it. All the bells and whistles that would have gone off if my pacemaker had actually discharged—none of them had. Just a dream. Just the melatonin, which the hospital dispensed in a form I can only describe as strangely effective.
I texted my mother and Niles at 1:44 in the morning anyway, because an hour later my mind was still racing and there was nothing else to do. I told them both the same thing: I will not miss carrying this thing in my chest.
Two days earlier, I had been officially listed for transplant. I was Status 2 at The Christ Hospital in Cincinnati, on an Impella heart pump, waiting. The nightmare was just a nightmare. I knew that.
What I didn’t know was that by the end of the following day, I’d have a much more concrete basis for comparison.
The Weekend Curse
It had followed me to TCH.
The pattern had started weeks before my transfer—so reliable it had become almost darkly comedic. Friday night into Saturday, like clockwork, my heart would break from sinus rhythm into atrial fibrillation. The ER at Mercy West had seen it. The floor at TCH had seen it. I’d been cardioverted, medicated, and monitored through enough of these episodes that I no longer needed the monitor to tell me when one was starting. I could feel it—a particular flutter, a shift in pressure, something that preceded the alarms by enough time that the nurses had stopped running. They’d walk into the room and ask, “you feel that?” I’d say yes. We’d go from there.
Sunday evening, October 13th—two days after listing—it came back. The room filled up: crash cart, pads, the assembled response that the staff executed with the practiced calm of people who had done this many times. They managed it pharmaceutically this time. The rhythm corrected. The room cleared.
I texted my mother: I thought we had escaped the weekend curse.
She said she had too.
I told the nurses and doctors that if they killed me, I’d be back to haunt every last one of them—Halloween was right around the corner, and everyone knows the veil is at its thinnest then. They laughed. I think they appreciated the spirit of it. By that point they had a reasonable sense of the kind of patient they were dealing with.
The Long Monday
I woke the next morning still in it.
I had been in AFib most of the night, presenting a sinus rhythm for stretches, then slipping back. When I stood to urinate, my heart rate shot up. That was when they confirmed it: they were going to cardiovert.
Then they decided to try beta blockers first.
Then they waited on blood work.
Then they waited on my blood thinner levels—there’s a stroke risk with cardioversion, and they wanted me in therapeutic range before they fired the defibrillator. A heart rhythm specialist came in. He agreed cardioversion was the right call. They kept finding reasons to delay it.
I had been in AFib for going on twenty-two hours by the time afternoon arrived. This was the worst of the bouts—worse than anything at Mercy West, worse than anything in the weeks prior. I was wrung out. The room had more people in it than usual. They were bringing in a “VIP swan” catheter, running me down to the cath lab, preparing for what came next.
My family came up while all of this was going on.
I had told the staff not to let them back. I didn’t want them to see me like that. The staff let them back anyway.
I was flat on the bed. I looked, by every account including my own, like a man who was not going to make it. I told them it looked worse than it actually was. I don’t think that helped. They stood in that room and looked at me, and I could see what they were seeing.
I told the kids—and I chose my words with the particular care of a man who isn’t certain he’ll be having future conversations—that I expected to live. But if something went wrong, if things went south in ways none of us could predict, there was one thing I wanted for them. They hadn’t been raised with any religion. I’d always been uneasy about that. I’m not a man who has much use for organized religion in the institutional sense, but I believe, with some conviction, that a spiritual practice of some kind is not optional. That it matters. I told them to find one.
Then they sent my family out and brought in the defibrillator.
The Baseline
I want to establish something first.
I am not a man who lacks reference points for electrical shock. As a child, I did what curious children sometimes do near an open outlet—I introduced a screwdriver to it. The result was instructive. Later, in law enforcement training, our instructor lined us up with a handheld taser, the kind with two prongs you press against someone and discharge. He gave us a choice: arm or leg. When I reached him, I said leg. He zapped my arm anyway. I said, ouch, dammit, I said the leg. He said, oh, sorry, and promptly zapped my leg too. The class—instructor included—found this hilarious. So did I, eventually.
These were real experiences of electrical shock. They were not theoretical. I knew what it felt like.
They were nothing.
The Hit
The anesthesiologist on duty that day was not Dr. Judah, who had developed what he called a ketafol cocktail—a combination of ketamine and propofol—that had worked reliably through earlier procedures. This doctor had his own version. It had worked well enough for what came before. It did not work well enough for what came next.
I heard the defibrillator charging. The pitch of the hum rose as the charge built. I was immobilized—fully under in every physical sense, unable to move, unable to speak. I was also, with complete clarity, awake.
I yelled that I was awake. Nothing came out.
The charge kept building.
Holy shit, they don’t know I’m awake. This is going to hurt like hell.
Then came the clear. Then came the hit.
Two horses—one in front, one behind—kicking me in the chest nearly simultaneously. My body convulsed. I yelled again, silently, with everything I had. Not in panic. In anger and in pain.
It corrected the arrhythmia.
When I came fully out of it shortly afterward, I told them I had been alert for all of it. They apologized. There was nothing to be done about it by then. It was over. I had survived it. And as brutal as it was—brutal in a way I lack adequate language for—it wasn’t even the worst thing that had happened to me by that point in the hospitalization. That fact alone says something about the preceding weeks.
I should note the ketamine, because it belongs here even if it belongs more fully to another piece. Dr. Judah’s cocktail had been part of earlier procedures, and ketamine does something that straight sedation does not: it separates. Consciousness lifts away from the body. On one of those earlier occasions I found myself flying around the room—above the heads of the staff, the equipment, everything—hearing conversations happening twenty feet from the bed and able to repeat them back afterward. I was a spectator at my own procedure. Chemistry, not mysticism. Still—a reminder of how thin certain lines can be.
The Rebound
The right ventricle had been failing.
By late that Monday, the situation had deteriorated enough that the team was discussing an RVAD—a right ventricular assist device, one step removed from ECMO, which is essentially a bypass of everything. They were preparing to insert it in the morning.
The right ventricle held overnight.
No surgery. When they told me Tuesday morning, I had already lost nearly seven pounds of fluid they’d pulled off me in the night. I did two laps around the ward. Two—where three had been easy just days before. I felt the difference. The second lap was a push.
But I was upright. I was moving.
The Quiet Weekend
Dowling had a theory about the AFib.
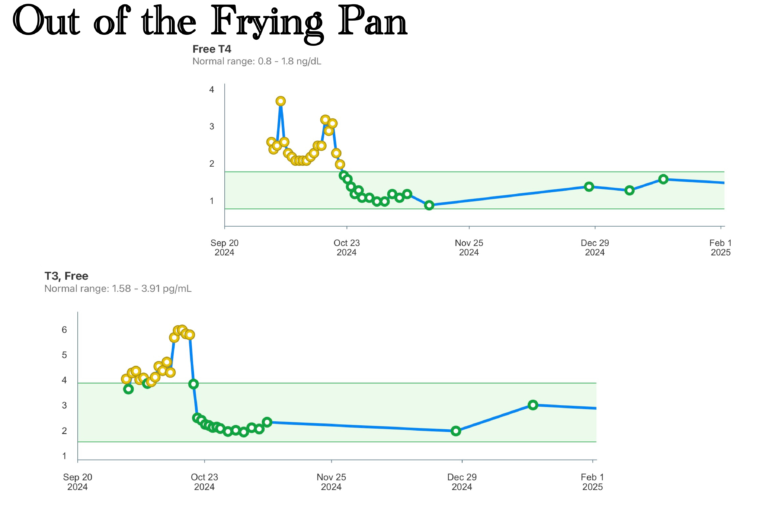
He’d been saying it for days: the thyroid was the accelerant. The amiodarone I’d been on for years—thirty-seven percent iodine by weight, lipophilic, with a half-life measured in months—had saturated my thyroid tissue and driven it into a state of toxic overproduction. The hormones it was dumping into my system were throwing my heart into chaos on a schedule so regular it had come to feel like a law of nature. Remove the thyroid, he believed, and the pattern would break.
The thyroidectomy was October 19th. That’s its own piece.
What belongs here is what happened the following weekend.
It didn’t come.
Saturday passed. Sunday passed. The crash cart stayed in the hallway. The nurses walked in to check on me and walked back out. No flutter. No shift in pressure. No moment of recognition before the alarms. The weekend curse that had defined six consecutive weeks of my life simply failed to materialize.
I texted my mother at 5:35 on the Monday morning after: Quiet night; nothing to report. I maintained rhythm through the night.
She told me to stay that way.
I intended to.
The mini bug zapper—the one I’d been carrying in my chest for twenty years—stayed quiet through the whole ordeal. The real one, the one they wheeled into the room, did the work instead. I am told this is not unusual. I’m not convinced.
Discover more from One More Beat
Subscribe to get the latest posts sent to your email.




Good Lord, what an ordeal you’ve been through. You write about it well, with good storytelling rhythm. But holy wow what a story.