Dignity
There is a transaction that occurs the moment you are admitted to a hospital for a serious, extended stay. Nobody explains it to you in advance. Nobody sits down and walks you through the terms. It simply happens, quietly and completely, from the first hour.
You surrender agency over your own body.
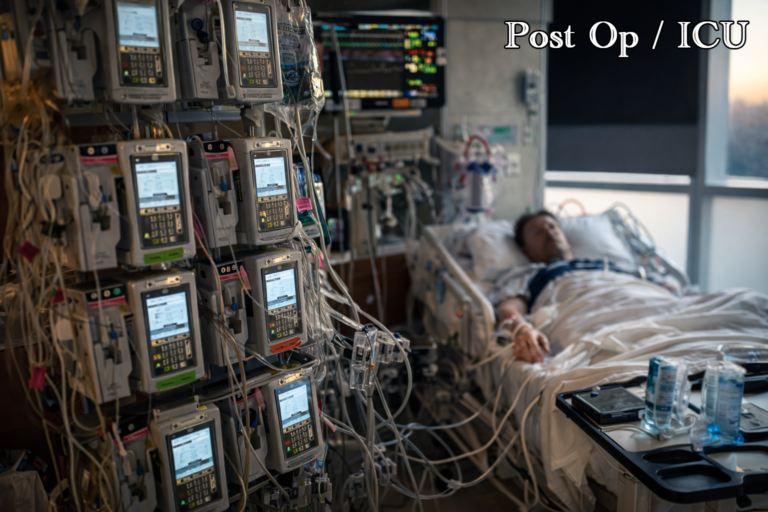
Not partially. Not temporarily in some abstract, philosophical sense. Completely. Every input is measured, every output logged. You do not eat without it being recorded. You do not move without assistance or permission. You do not clean yourself without help. The body you have inhabited and managed your entire adult life becomes, for the duration, a clinical object—monitored, maintained, and managed by other people around the clock.
This is not cruelty. It is medicine. The monitoring is what keeps you alive. The management is the point.
The cost is real, and it accumulates quietly.
What Goes First
The foley catheter handles urination for as long as it is in place. When it comes out, the bedside commode takes over—a chair with a receptacle, positioned within reach of the bed, because the bathroom across the room is too far and the walk too risky and everything, in any case, must be measured.
Everything.
Urine in a receptacle, volume logged. Every bowel movement in the commode, weighed and recorded. The body reduced to inputs and outputs, tracked with the same clinical precision as the cardiac monitor and the Impella readings. You understand why. You accept why. Understanding and acceptance do not make it easier.
The first time someone else has to wipe you is its own experience. There is no graceful way to describe it and no point in trying. You are an adult who has managed your own body for decades, and now you cannot. The particular humiliation of that moment is real. What is also real is the particular grace required of the person doing it—the matter-of-fact professionalism that says this is part of the care, not a comment on you. The staff at TCH (The Christ Hospital) had that grace. It did not make the moment comfortable. It made it survivable.
The Line I Held
There was one place I would not move.
When the foley came out and the commode took over, I was physically capable of handling the cleanup myself. Weak, yes. Attached to lines, yes. But physically capable. And I refused.
Not out of stubbornness for its own sake. Out of a standard I was not willing to drop: I would not handle myself and then not wash my hands. That was the line. Simple, non-negotiable, mine.
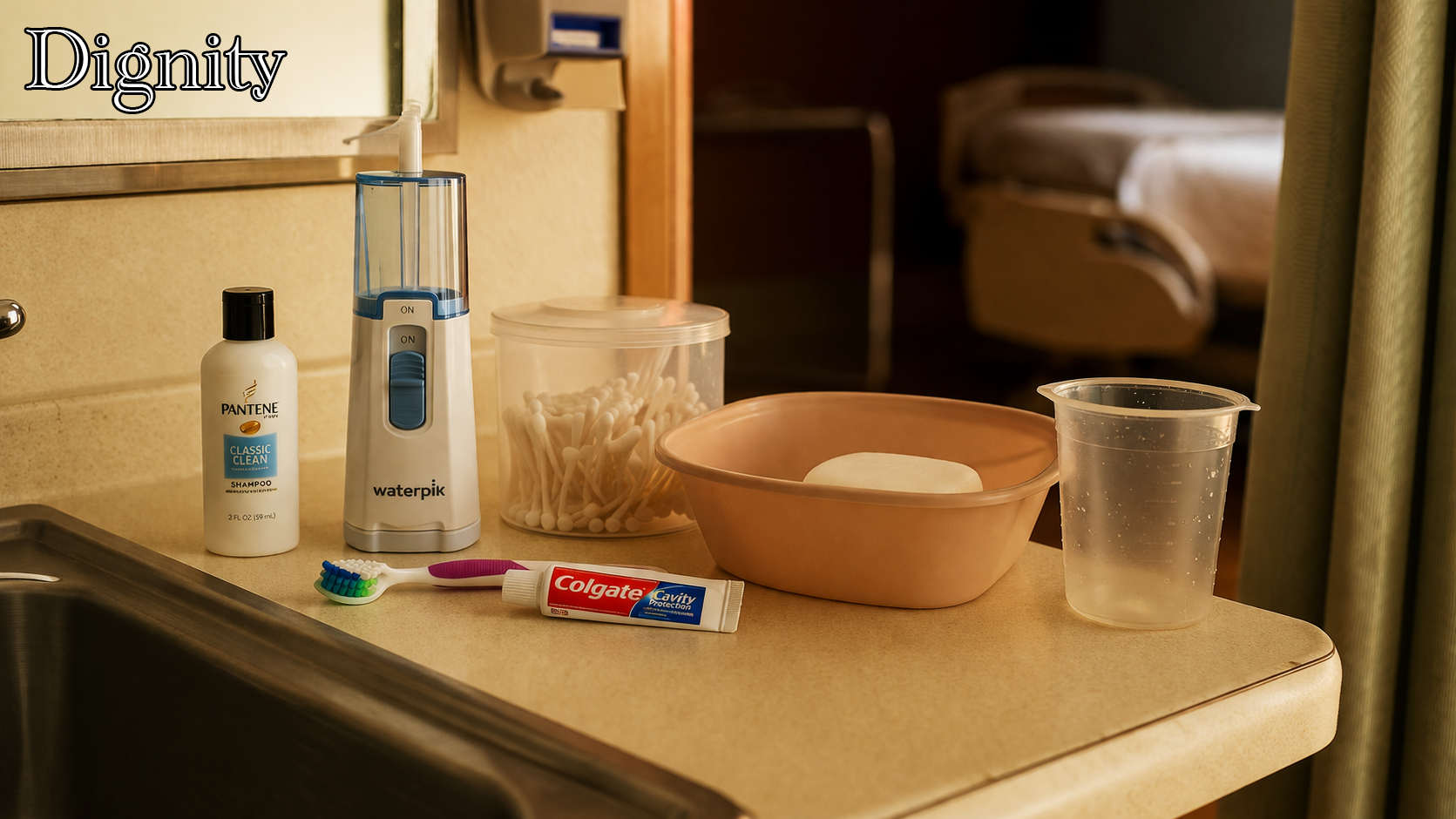
Getting the line respected took negotiation. The solution—a basin, soap, a container of water poured over my hands into the basin bedside—was not complicated. It cost the staff thirty seconds. It cost me nothing except the advocacy required to get there. But it mattered in a way that is difficult to explain to someone who has not been in that position. When almost everything has been taken, the things you manage to keep carry disproportionate weight.
Eventually, they allowed me access to the sink in the corner of the room. That was a different level entirely. The sink meant I could wash my hands properly. It meant I could brush my teeth at a sink like a person, not a patient. It meant a small but genuine restoration of the ordinary.
I had been brushing twice daily before admission—manual brush, electric brush, WaterPik with Listerine for irrigation. That routine is not vanity. For a patient heading into major surgery, with heavy immunosuppression on the horizon, oral hygiene is clinical. Letting it lapse was not an option I was willing to consider. Getting to the sink, and getting Ashley to bring vinegar so I could properly clean the WaterPik and CPAP, restored a routine that mattered medically as much as it mattered personally.
Ashley brought the vinegar on her own initiative. Nobody asked her.
Sam, Mel, and Ash
Thomas got his moment earlier in this series—the former 82nd Airborne nurse who told me transplant was a covenant and meant every word of it. There were others who earned their moment. Three of them belong here.
Melanie was on shift when they needed one more blood draw—a fresh stick, they insisted, no exceptions. By that point in the hospitalization my skin had become extraordinarily sensitive from the accumulated trauma of weeks of procedures, and they wanted the hand. I fought that. Hard. Melanie didn’t argue. She assessed, found a vein on the top of my forearm—and I have excellent veins, the kind of target a blind man could hit—and drew the vial without my feeling it. Then, without being asked, she walked me through a desensitization exercise: simply rubbing the skin, methodically, over the sensitized area. The technique works by re-establishing normal sensory input to skin that has been overstimulated into hyperreactivity—essentially resetting the nervous system’s response to touch in that region. It also helps with anxiety. She did not have to do either of those things. She did them anyway.
Ashley was a constant. When I needed vinegar for the WaterPik and CPAP, she brought it. When I mentioned, offhandedly, that TCH was a Pepsi institution and what I actually needed—desperately, in the particular way one craves a specific comfort under sustained stress—was the burn of a Coca-Cola at the back of the throat, she Door Dashed two twelve-packs—one each of regular and Diet Coke—bought on her own dime.
The gesture was small. The impact was not. When everything around you is institutional and managed and clinical, a twelve-pack of Diet Coke bought by a nurse out of her own pocket lands like something else entirely. It lands like being seen.
Sam was the night shift regular toward the end of my pre-transplant time in the ICU. She was the one who suggested I could wash my hair in the sink if I was careful about it—a thought that had not occurred to me and that, once suggested, became immediately, urgently necessary. She was also the one who sat with me the night before the transplant and worked through the mechanics of intubation and extubation—the part of the procedure I had the most questions about, the part nobody had fully explained to my satisfaction until she did. That story belongs in the next piece. What belongs here is that she was present, consistently, in the hours when the ward was quiet and the night was long and the mind went where it wanted to go.
Soap and Water
Mom brought the shampoo.
I had been using the dry shampoo cap the hospital provided—a heated cap that is supposed to clean hair without water. After nearly a month, it had ceased to do anything detectable. I texted Mom on the morning of October 26th and asked for a small travel bottle of shampoo. She brought it that afternoon.
That evening, Sam suggested the sink.
I leaned over it and she helped work the shampoo through. The water ran dark. An amount of accumulated material that I will charitably describe as significant went down the drain over the next several minutes. When it was done I stood up and my hair was clean—actually clean, separate strands, moving individually the way hair is supposed to move.
I texted Niles: I actually have separate hairs on my head again.
He understood immediately.
The Q-tips were next on the list. The hospital provided long cotton swabs that were not the same, and after the hair washing I had attempted to clean my ears and confirmed they were not the same. I asked Mom to bring proper ones on her next visit. She did.
There is something ancient about washing another person’s hair. It requires trust at a level most human interactions don’t reach—a surrendering of the head, which is where we locate the self. The act is intimate in a way that transcends the clinical. The word for it, in older traditions, is ablution: ritual washing, the crossing of a boundary. Before and after. The water carries something away that isn’t just dirt.
I went to bed that night with clean hair, Sam changing my Impella dressing with the quiet efficiency she always brought to it, the ward settling into its overnight rhythm.
Nothing had changed in the large sense. The room was the same room. The lines were the same lines. The monitor glowed the same green behind my head.
But I had separate hairs. The WaterPik was clean. And for that night, in that room, that was enough.
What Small Things Do
The Diet Coke. The vinegar. The basin. The shampoo. The Q-tips.
None of these things are dramatic. None of them appear in any clinical protocol or care plan. They are the things that exist in the space between medicine and humanity—the things that cannot be ordered or charted or measured, yet sometimes matter enormously to the person in the bed.
When almost everything has been taken, the return of anything is disproportionate. This is not sentiment. It is arithmetic.
If you are supporting someone through a long hospitalization, you cannot restore what hospitalization takes. But you can bring that one thing. The specific comfort. The small ordinary pleasure that has been lost.
Bring the shampoo. Bring the Q-tips. Show up with the Diet Coke.
It lands differently.
Discover more from One More Beat
Subscribe to get the latest posts sent to your email.